According to data from the Australian Bureau of Statistics (2025), 14.2% of Australians over the age of 18 and 44.7% of those aged over 75 were displaying indicators of chronic kidney disease (CKD) in 2022-2024.
Of those displaying indicators of CKD, 99% were showing early stages (stages 1 to 3) of the disease (ABS 2025).
CKD appears to be highly underdiagnosed, with the same data suggesting that among those displaying indicators of CKD, only 7.4% self-reported having the condition (ABS 2025).
This is likely because CKD is a ‘silent’ illness that characteristically causes few or no symptoms, sometimes until 90% of kidney function has already been lost (Better Health Channel 2018).
Luckily, CKD is a mostly preventable condition because many of its risk factors are modifiable (Healthdirect 2023).
What is Chronic Kidney Disease?

Kidney Health Australia (2024) defines CKD as either one of the following:
- An estimated or measured glomerular filtration rate (GFR) of less than 60 mL/min/1.73m2 that is present for ≥ three months with or without evidence of kidney damage, or
- Evidence of kidney damage with or without decreased GFR that is present for ≥ three months, as evidenced by the following:
- Albuminuria
- Haematuria after exclusion of urological causes
- Structural abnormalities (e.g. on kidney imaging tests)
- Pathological abnormalities (e.g. renal biopsy).
What Causes Chronic Kidney Disease?
The kidneys, which are located on each side of the backbone below the ribs, are two organs responsible for filtering waste from the blood and excreting it via urine (Healthdirect 2024).
If the kidneys are damaged and not functioning properly, fluid and waste accumulate in the body instead of being expelled (Healthdirect 2023). This may lead to a variety of complications such as hypertension, anaemia, weak bones, poor nutrition and nerve damage. If CKD continues to progress, it may eventually lead to kidney failure, requiring the patient to undergo dialysis or a kidney transplant (NKF 2023).
The most common cause of CKD in Australia is diabetes, which accounts for about one-quarter of cases. This is known as diabetic nephropathy and occurs when high levels of blood sugar damage the glomeruli (filtering units in the kidneys) over time, impairing their ability to filter waste (Healthdirect 2023; NKF 2023).
CKD can also be caused by:
- Hypertension
- Glomerulonephritis (inflammation of the glomeruli)
- Interstitial nephritis (inflammation of the tubules and surrounding structures in the kidneys)
- Polycystic kidney disease, which causes large cysts to form and damage kidney tissue
- Congenital abnormalities in the urinary tract
- Certain autoimmune conditions, including lupus nephritis, which causes inflammation of the glomeruli
- Obstructions of the urinary tract (e.g. kidney stones or tumours)
- Enlarged prostate gland
- Recurrent urinary tract infections
- Vesicoureteral reflux - a condition causing urine to flow backwards into the kidneys.
(NKF 2023; Mayo Clinic 2023)
Risk Factors for Chronic Kidney Disease
Risk factors for CKD include:
- Diabetes
- Hypertension
- Cardiovascular disease
- Family history of kidney failure
- Obese (body mass index of 30 or higher)
- Past/current smoking and/or vaping
- Being over 60 years of age
- Being of Aboriginal or Torres Strait Islander origin and over the age of 18
- History of acute kidney injury (AKI).
(Kidney Health Australia 2024)
Aboriginal and Torres Strait Islander people are twice as likely to experience CKD as non-Indigenous people, have an earlier age of disease onset and experience faster disease progression. This has been linked to the ongoing effects of colonisation (Kidney Health Australia 2024).
Symptoms of Chronic Kidney Disease
There are typically few or no symptoms in the early stages of CKD. In later stages, the patient may experience:
- Hypertension
- Changes in the frequency and quantity of urine, particularly at night (e.g. waking up to urinate)
- Changes in urine appearance (e.g. frothy or foaming)
- Haematuria (blood in the urine)
- Swelling in the legs, ankles or around the eyes
- Pain in the kidney area (back, under the lower ribs)
- Pain or a burning sensation when passing urine
- Fatigue and lethargy
- Reduced appetite
- Headaches
- Difficulty concentrating
- Itchiness
- Shortness of breath
- Nausea and vomiting
- Bad breath and a metallic taste in the mouth
- Pins and needles in fingers or toes
- Restless legs
- Feeling generally unwell
- Sleeping difficulties.
(Healthdirect 2023; Better Health Channel 2022; NKF 2023)
Complications of Chronic Kidney Disease
CKD can cause a variety of complications, including:
- Anaemia - the kidneys are responsible for producing the hormone erythropoietin (EPO), which is involved in red blood cell production. Someone with kidney disease cannot produce an adequate amount of EPO, and subsequently, red blood cells
- Hyperkalaemia (high levels of potassium)
- Fluid retention, which may lead to oedema in the arms and legs, hypertension or pulmonary oedema
- Heart disease
- Increased bone fragility and risk of fractures
- Reduced sex drive, erectile dysfunction or decreased fertility
- Central nervous system damage, leading to concentration issues, personality changes or seizures
- Reduced immune function
- Pericarditis
- Pregnancy complications.
(Healthdirect 2023; Mayo Clinic 2023; NKF 2015)
How is Chronic Kidney Disease Diagnosed?
There are three essential components to diagnosing CKD:
- Estimated glomerular filtration rate (eGFR) (to determine the kidney function stage)
- Urine albumin-to-creatinine ratio (uACR) (to determine the level of albuminuria)
- Underlying pathology testing (to determine the cause of CKD).
(Kidney Health Australia 2024)
A routine Kidney Health Check comprising a blood pressure measurement, uACR and eGFR should be offered annually for patients who:
- Have diabetes
- Have hypertension
- Are of Aboriginal or Torres Strait Islander origin and over the age of 18.
(Kidney Health Australia 2025)
Patients with any other risk factors should be offered a routine Kidney Health Check every two years (Kidney Health Australia 2025).
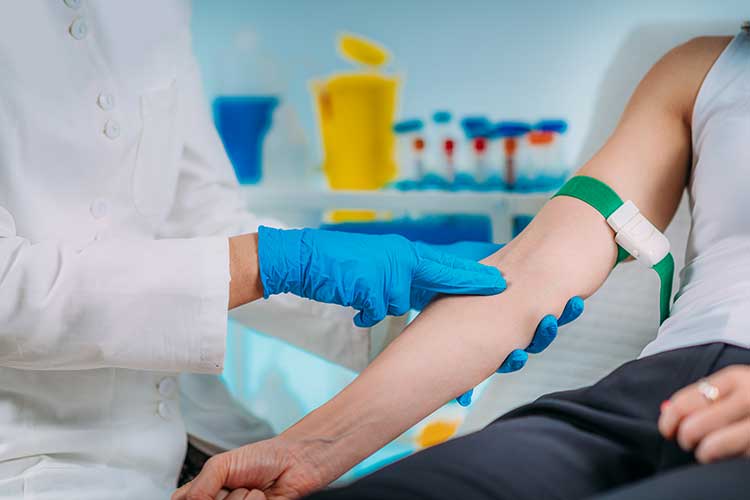
An eGFR involves taking a blood sample from a vein in the arm, which is then used to calculate how well the kidneys are filtering certain agents produced by the body. Typically, it involves measuring creatinine levels in the blood (NKF 2022).
If the patient returns an abnormal eGFR result (< 60 mL/min/1.73m2), the test should be performed again within seven days. If there is a further ≥ 20% reduction in eGFR, this may indicate acute kidney injury. However, if the eGFR is still reduced but stable, the test should be repeated again within three months. If at least two of these tests show reduced eGFR, this is an indication of CKD (Kidney Health Australia 2024).
If the patient returns an abnormal uACR result (≥ 3 mg/mmol), the test should be performed again within the next three months. If the second test shows a normal uACR result, a third test should be performed (ideally the first morning void). If at least two of these tests show an elevated uACR, this is also an indication of CKD (Kidney Health Australia 2024).
The patient’s eGFR and uACR can then be combined:
| Albuminuria Stage | ||||
| Kidney Function Stage | GFR | Normal uACR < 3.0 mg/mmol |
Microalbuminuria uACR 3.0-30 mg/mmol |
Macroalbuminuria uACR > 30 mg/mmol |
| 1 | ≥ 90 | Not CKD unless haematuria, structural or pathological abnormalities present | ||
| 2 | 60-89 | |||
| 3a | 45-59 | |||
| 3b | 30-44 | |||
| 4 | 15-29 | |||
| 5 | < 15 or on dialysis | |||
(Adapted from Kidney Health Australia 2024)
Each coloured area (yellow, orange or red) requires a different management strategy. For more information, see Kidney Health Australia’s guidelines on Chronic Kidney Disease (CKD) Management in Primary Care.
Once the patient’s kidney function stage and albuminuria stage have been identified, further investigations to determine the underlying cause of the CKD will need to be performed (Kidney Health Australia 2024).
These may include:
- Blood pressure assessment
- Other blood tests
- Imaging (e.g. ultrasound, CT scan)
- Biopsy.
(Better Health Channel 2022; Healthdirect 2023)
Managing Chronic Kidney Disease
First-line management for CKD is lifestyle modification, including:
- Weight loss (BMI should ideally be < 25, or < 23 in Asian people)
- Smoking/vaping cessation
- Increasing physical activity
- Limiting alcohol intake
- Ensuring adequate nutrition
- Treating underlying conditions (e.g. hypertension, diabetes, high cholesterol, urinary tract infection)
- Medication review (some medicines can affect the kidneys).
(Kidney Health Australia 2024; Healthdirect 2023)
In stages 3 or 4, the patient may require additional medicines or adjusted dosages and possibly a referral to a nephrologist if indicated. Symptoms or complications should be addressed as appropriate (Kidney Health Australia 2024; Healthdirect 2023).
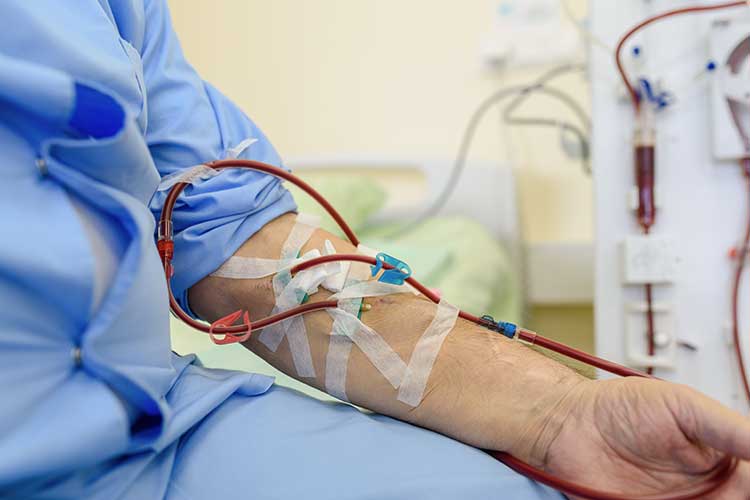
In stages 4 or 5, the kidneys may be unable to function on their own. Once the kidneys fail, the patient will require renal replacement therapy (dialysis and/or a kidney transplant). They may also receive supportive care (Kidney Health Australia 2024; Healthdirect 2023).
Preventing Chronic Kidney Disease
CKD is a largely preventable condition. The risk can be reduced by making lifestyle changes, including:
- Maintaining a healthy weight
- Maintaining a healthy diet
- Drinking adequate water
- Exercising regularly
- Avoiding smoking and vaping
- Limiting alcohol
- Reducing stress
- Undergoing routine kidney checks if any risk factors are present.
(Healthdirect 2023)
Test Your Knowledge
Question 1 of 3
Why is chronic kidney disease often underdiagnosed?
Topics
Further your knowledge
References
- Australian Bureau of Statistics 2025, National Health Measures Survey, Australian Government, viewed 1 May 2025, https://www.abs.gov.au/statistics/health/health-conditions-and-risks/national-health-measures-survey/latest-release#chronic-kidney-disease
- Better Health Channel 2022, Kidney Disease, Victoria State Government, viewed 1 May 2025, https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/kidney-disease
- Healthdirect 2023, Chronic Kidney Disease, Australian Government, viewed 1 May 2025, https://www.healthdirect.gov.au/chronic-kidney-disease
- Healthdirect 2024, Kidneys, Australian Government, viewed 1 May 2025, https://www.healthdirect.gov.au/kidneys
- Kidney Health Australia 2024, Chronic Kidney Disease (CKD) Management in Primary Care, 5th edn, Kidney Health Australia, viewed 1 May 2025, https://kidney.org.au/health-professionals/ckd-management-handbook
- Kidney Health Australia 2025, Do You Need a Kidney Health Check?, Kidney Health Australia, viewed 1 May 2025
- Mayo Clinic 2023, Chronic Kidney Disease, Mayo Clinic, viewed 1 May 2025, https://www.mayoclinic.org/diseases-conditions/chronic-kidney-disease/symptoms-causes/syc-20354521
- National Kidney Foundation 2015, Anemia and Chronic Kidney Disease, NKF, viewed 1 May 2025, https://www.kidney.org/atoz/content/what_anemia_ckd
- National Kidney Foundation 2022, Estimated Glomerular Filtration Rate (eGFR), NKF, viewed 1 May 2025, https://www.kidney.org/atoz/content/gfr
- National Kidney Foundation 2023, Chronic Kidney Disease (CKD) Symptoms and Causes, NKF, viewed 1 May 2025, https://www.kidney.org/atoz/content/about-chronic-kidney-disease
 New
New 

