Caring for Enteral Tubes
Published: 15 June 2023

Published: 15 June 2023

Up 40% of hospitalised patients in Australia are affected by malnutrition (ACSQHC 2018).
Without nutritional support, these patients may deteriorate, leading to poor outcomes such as prolonged hospital stays, infection and compromised recovery (DAA 2018).
Enteral feeding is the delivery of liquid nutritional support through a tube inserted into the gastrointestinal tract. It is used for patients who are unable to meet their nutritional requirements through oral intake. This may be because:
(Dietitians Australia 2023)
Enteral feeding may complement oral intake or be used completely in place of oral intake (Dix 2018).
Enteral feeding is considered for patients who:
(Adeyinka et al. 2022)
Patients with the following conditions may require enteral feeding:
(Adeyinka et al. 2022; Dietitians Australia 2023; Complex Nutrition Working Group 2019)
If the patient’s gastrointestinal tract is compromised (e.g. gut failure or intestinal obstruction) or inaccessible via an enteral tube, they may require parenteral nutrition instead. This involves nutrients being inserted directly into the bloodstream via a central venous catheter (Adeyinka et al. 2022; Dietitians Australia 2023).
Older adults or patients receiving palliative or end-of-life care may not be suitable for enteral feeding. You should take into account quality of life, possible complications and expected outcomes when making a decision (DAA 2018).
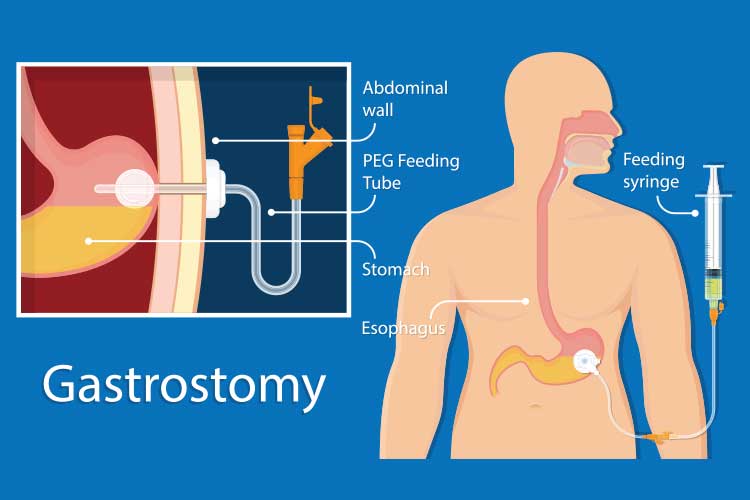
There are three sites on the body where an enteral feeding tube can be inserted, and several types of tubes that can be used, each taking a different route. This will depend on:
(DAA 2018)
| Site | Route Options |
| Gastric (stomach) |
|
| Duodenum (small intestine) |
|
| Jejunum (small intestine) |
|
(Adapted from WACHS 2019)
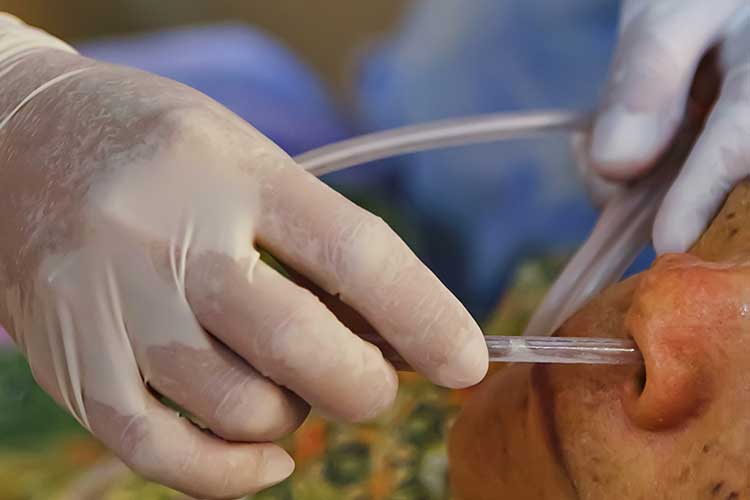
Before the commencement of feeding, you must ensure the tube is positioned correctly. Poor placement or tube migration can cause potentially life-threatening aspiration of feed (DAA 2018).
Placement must be confirmed through x-ray and/or by measuring the pH level of gastric aspirate (refer to your facility’s policies and procedures). A pH of less than 5.5 generally indicates that the tube is correctly positioned in the stomach (WACHS 2019).
Other methods of confirming placement are not recommended as they are less accurate (DAA 2018).
Tube placement should be assessed:
(WACHS 2019)
In addition to ensuring the tube is correctly positioned, you can also minimise the risk of aspiration by:
(Souza 2018; CDHB 2022)
Caring for enteral tubes may include:
(WACHS 2019)
When caring for a patient with an enteral tube, it is important to regularly monitor the following:
(Bapen 2016; WACHS 2019)
Note: Refer to your organisation’s policies and procedures for the required frequency of monitoring.
Possible complications of enteral feeding include:
(Adeyinka et al. 2022)
Enteral feeding is important for providing nutritional support but can be dangerous if performed incorrectly. In order to avoid potentially life-threatening complications, correct and thorough care of the feeding tube is essential.
Note: This article is intended as a refresher and should not replace best-practice care. Always refer to your facility's policy on managing enteral feeding.
Question 1 of 3
True or false: Enteral tube placement must be confirmed before feeding commences.