Dialysis Basics
Published: 23 March 2022
Published: 23 March 2022

The kidneys are responsible for filtering waste from the blood and excreting it via urine. However, when the kidneys become damaged, such as in the case of renal failure, they are unable to filter waste properly, causing it to accumulate in the blood (Healthdirect 2020). This is a potentially life-threatening complication (NHS 2021).
Dialysis is a treatment used to artificially filter waste from the blood if the kidneys are no longer able to do so on their own (Healthdirect 2020). While dialysis isn’t a cure for renal failure, it’s a type of supportive care that can sustain the patient until they can receive a kidney transplant, or for the rest of their life if a transplant is contraindicated (NHS 2021).
In the case of acute renal failure, dialysis can be used until the kidneys recover (NHS 2021).
Specifically, the role of dialysis is to:
(NKF 2022)
Dialysis is typically required once a patient enters end-stage renal failure: that is, when 85 to 90% of kidney function has been lost and their glomerular filtration rate (GFR) is under 15 (NKF 2022).
There are two types of dialysis:
(Healthdirect 2020)
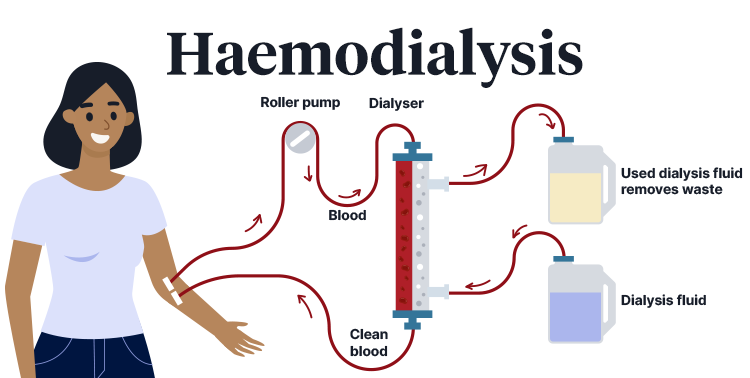
Haemodialysis, which is the most common type of dialysis, involves filtering blood through an external device known as a dialyser (NIDDK 2018).
The procedure involves gaining vascular access to the patient’s arm or leg (either via a fistula, graft or catheter) and drawing blood into a tube connected to the dialyser. The blood is then filtered through the dialyser before being circuited back into the patient’s bloodstream. Only a small amount of blood is outside of the patient’s body at one time (Better Health Channel 2019).
The process takes about four to five hours and needs to be performed at least three times per week (Better Health Channel 2019).
Haemodialysis can be performed at a haemodialysis unit or satellite centre, or in the patient’s home, providing they have the appropriate equipment (Better Health Channel 2019).
Home haemodialysis is generally preferred as it allows the patient to tailor their treatment schedule to their needs (e.g. while they are sleeping) and receive dialysis more frequently, which will improve their health (Better Health Channel 2019).
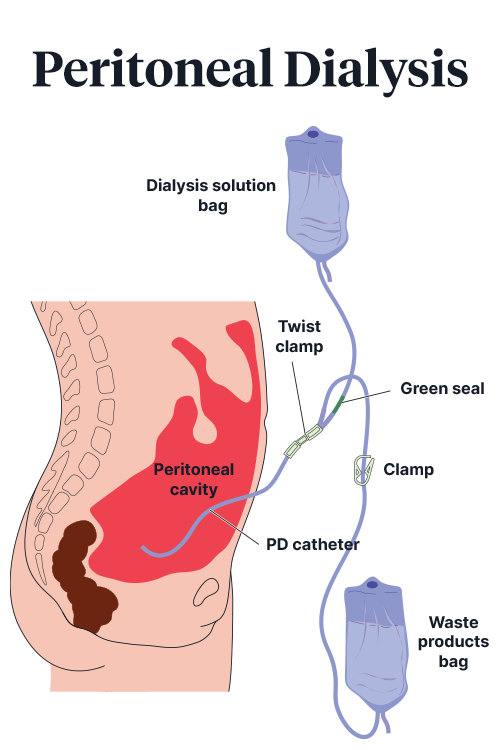
Rather than employing an external device, peritoneal dialysis involves using the peritoneal membrane - the lining of the abdominal cavity - as an internal filter (Better Health Channel 2019).
In order to perform peritoneal dialysis, a catheter needs to be inserted into the peritoneal cavity, where it will stay in situ as long as the patent requires dialysis (Better Health Channel 2019).
A cleansing solution (dialysate) is pumped into the body via the catheter, where it absorbs the waste products that have been filtered out of the blood by the peritoneal membrane. The dialysate, now containing the waste, is then drained back out of the body and into a bag and replaced with fresh dialysate (Mayo Clinic 2021; NHS 2021).
Each cycle of filling, draining and replacing the peritoneal membrane with dialysate is known as an exchange. There are two different schedules of exchange that may be used:
(Better Health Channel 2019)
In most cases, both types of dialysis are equally effective and the chosen method will depend on the patient’s preference and lifestyle (NHS 2021).
However, there are certain circumstances where a particular type of dialysis might be preferred:
| Haemodialysis may be preferred for: | Peritoneal dialysis may be preferred for: |
|---|---|
|
|
(NHS 2021)
There are also a variety of pros and cons to consider for each type of dialysis:
| Haemodialysis | Peritoneal dialysis | |
| Pros |
|
|
| Cons |
|
|
(NHS 2021; NKF 2021; NIDDK 2018)
Both types of dialysis can cause side effects. These may include:
(NHS 2021; Cleveland Clinic 2021; NIDDK 2018)
Patients who are undergoing haemodialysis should undergo blood testing once per month to ensure that any required adjustments to their dialysis prescription can be made. Furthermore, they should be weighed before and after each treatment, and monitor their own weight at home, to ensure there is no accumulation of fluid between dialysis sessions (Berns 2021).
The vascular access site should also be monitored and cared for in order to prevent complications. Site care should include:
(Berns 2021)
Infection is one of the most serious potential complications of peritoneal dialysis. It’s crucial to know when to escalate care. Signs to look out for include:
(Burkart 2021)
Question 1 of 3
Overall, which type of dialysis is most effective?