Diabetic Retinopathy
Published: 23 May 2022

Published: 23 May 2022

Diabetic retinopathy is the most common cause of vision loss in Western working-age adults (Shukla & Tripathy 2021). In fact, among the 1.7 million Australians who have diabetes, about one-third are estimated to have some degree of diabetic retinopathy (CERA 2020).
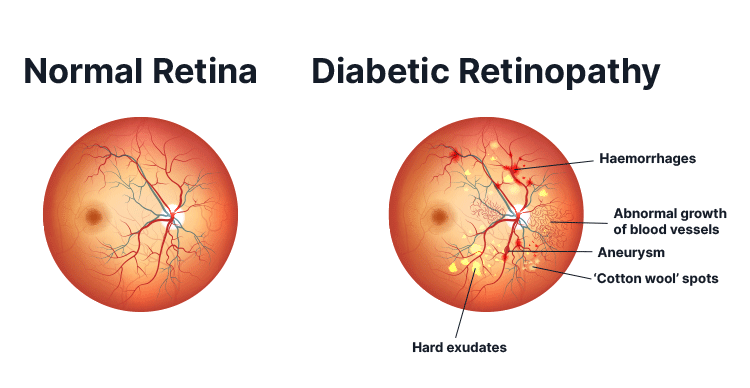
Diabetic retinopathy (DR) is a microvascular disorder caused by long-term diabetes, characterised by gradual vision-threatening damage to the retinal blood vessels (Shukla & Tripathy 2021).
If left untreated, DR can result in irreversible blindness (Dirani et al. 2013).
DR is associated with chronic hyperglycaemia and occurs when excess glucose obstructs the blood vessels in the retina, cutting off their blood supply (Shukla & Tripathy 2021; Mayo Clinic 2021).
There are two stages of DR:
(myDr 2018; Mayo Clinic 2021; Dirani et al. 2013)
Macular oedema, wherein fluid leakage from the retinal blood vessels causes swelling of the macula, can occur in any stage of DR. This may impair central vision, which is used for tasks such as reading and driving (Better Health Channel 2015; myDr 2018). Macular oedema is the most common cause of vision loss in diabetes (Dirani et al. 2013).
All people with type 1 and 2 diabetes are at risk of DR. However, effectively controlling diabetes reduces the likelihood (Vision Initiative 2021).
As a general rule, the longer the patient has had diabetes, the greater the risk of developing DR (CERA 2020).
Factors that might increase the risk of DR include:
(myDr 2018; Shukla & Tripathy 2021; Payne et al. 2012; Mallika et al. 2010; Rübsam et al. 2018)

There are typically no symptoms in the early stages of DR (CERA 2020). In advanced stages, patients might experience:
(Healthdirect 2020; CERA 2020; Vision Initiative 2021)
Potential complications of DR include:
(Mayo Clinic 2021)
Regular eye examinations, early diagnosis and treatment are essential to try to prevent severe vision loss. This includes a baseline eye examination when diabetes is first diagnosed (Better Health Channel 2015).
DR is diagnosed through an eye examination that typically comprises digital retinal photography and a dilated eye exam. In this exam, eye drops are used to dilate the eyes so that the practitioner can get a better view of the eye using a slit lamp or ophthalmoscope to examine for evidence of DR (CERA 2020; myDr 2018).
DR can’t be cured, but if detected early, management strategies can be used to prevent vision loss before any damage is done. If the patient has already experienced vision loss due to DR, treatment can stop it from worsening but may be unable to restore vision that has been lost (Diabetes Australia 2021; myDr 2018).
The best way to prevent vision loss is the effective management of diabetes, including:
(Dirani et al. 2013)
Treatment is typically indicated when DR is in a proliferative stage, or macular oedema is present. It might involve one or more of the following:
(CERA 2020; Dirani et al. 2013)
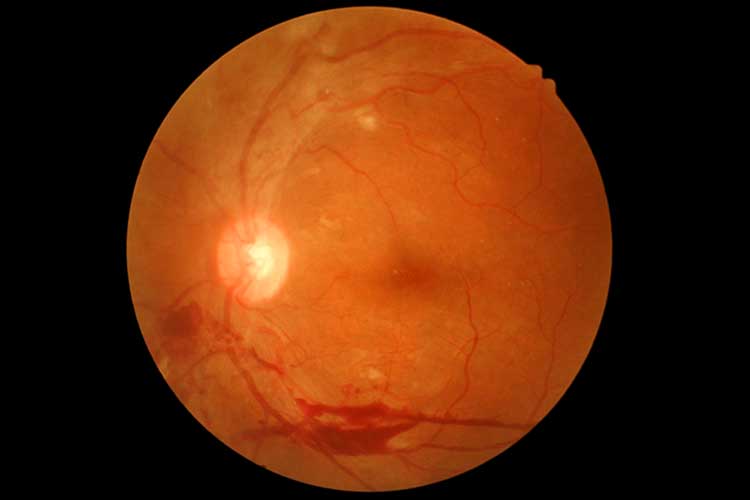
The best way to prevent vision loss from DR is for all people with diabetes to undergo regular eye examinations, as damage can usually be avoided if DR is detected early enough (CERA 2020).
It’s essential that people with diabetes undergo an eye examination:
(Vision Initiative 2021)
In order to increase the number of people with diabetes undergoing regular eye checks, Diabetes Australia and Vision 2020 Australia have established an eye check reminder program called KeepSight.
For more information, see KeepSight’s website.
Question 1 of 3
As a general rule, how often should people with diabetes undergo eye checks?